Subjective Assessment:
A 22 y/o white female presented to the office stating that her current contact lenses (ACUVUE ADVANCE Daily Wear disposable lenses) were fit approximately 2 months ago by another practitioner. Upon wearing these lenses she experienced ocular dryness throughout the lens wearing day, which was especially pronounced at the end of the day. Her eyes were red most of the time and she could not increase her wearing time beyond 6-8 hours comfortably. During the first month of contact lens wear she was able to comfortably wear lenses for 14-16 hours without complaint or irritation.
Objective Assessment:
Each eye was corrected to 20/20- at distance with a plano over-refraction. The lenses were geometrically centered over the line of sight and completely covered the corneal surface extended approximately 1.0 mm circumferentially over the limbus. External observation of the conjunctiva revealed 2+ conjunctival hyperemia (see Figure 1). Slit lamp examination of the corneal surface showed 2+ diffuse coalesced punctate staining with fluorescein (see Figure 2). Lissamine green staining of the conjunctival surface showed a distinct band of coalesced staining in an arc pattern about 1-2 mm from the corneal limbus associated approximately with the edge of the lens (see Figure 3). The tarsal plate demonstrated subtle papillary changes (see Figure 4).
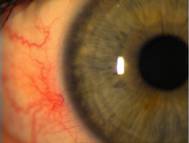
Figure 1 Conjunctival hyperemia - click to enlarge
|
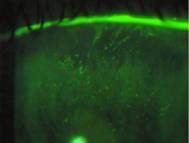
Figure 2 Diffuse coalesced punctate fluorescein staining - click to enlarge
|
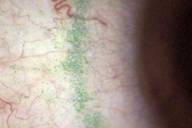
Figure 3 Lissamine green staining - click to enlarge
|
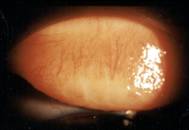
Figure 4 Upper tarsal conjunctiva - click to enlarge
|
Diagnostic Assessment:
Although several potential assessments were indicated by the signs and symptoms in this case, the most obvious differential diagnosis was between a true dry eye and contact lens-induced dry eye. The young age of this patient significantly ruled out true dry eye and argued in favor of contact lens-induced dry eye. However, other potential diagnoses were possible contributing factors. The presence of both corneal and conjunctival staining indicated a poor contact lens-to-cornea fitting relationship may have been a causative factor. While tarsal plate changes may imply an allergic component, these subtle papillary changes are also associated with mechanical irritation secondary to contact lens wear, as well as solution-related toxicity. Although not directly assessed in the slit lamp examination, systemic issues such as meibomian gland dysfunction and blepharitis can be causative factors in dry eye complaints and should be evaluated as a potential cause of lens-induced intolerance.
Additional questioning of this patient revealed she had recently changed from the original contact lens solution prescribed by the first practitioner. The patient had started her lens wearing experience using Opti-Free Express multi-purpose solution (MPS) and within the first month of lens wear had switched to a generic MPS brand.
Outcome:
Although signs and symptoms of this patient indicated dry eye to be a causative factor, her history revealed that the change in contact lens solution was likely to be the main culprit. Once the patient returned to the appropriate proprietary care system, her signs and symptoms resolved and she was able to return to full-time comfortable contact lens wear.
Discussion:
Fitting silicone hydrogel lenses is becoming rather commonplace around the world and is anticipated to eventually replace hydrogel lenses as the clinician’s lens of choice [1]. Clearly these materials offer patients improved physiological responses, whiter eyes, longer wearing times and generally fewer overall clinical complications for either daily or extended wear [2-4]. Since these materials are generally considered safer alternatives with fewer patient complications it is possible practitioners may assume that aftercare is no longer as important an aspect of the fitting process. While silicone hydrogel materials offer some unique physical differences from hydrogel materials, the clinical aftercare that is required to ensure patient success is not substantially different.
Contact lens care products are an often-overlooked cause of contact lens related intolerance and dry eye related symptoms. Some biguanide-preserved solutions have been associated with ocular stress as evidenced by increased corneal staining, redness, reduced wearing time and discontinuation of contact lens wear [5-7]. More recently end of day comfort has been associated with improved surface wetting indicating that differences exist in lens wettability for various storage solutions [8]. As a means to improve comfort, contact lens manufacturers are increasing the concentration of wetting agents within the polymer mix of some hydrogel and silicone hydrogel lens materials. For example, ACUVUE OASYS has twice the concentration of HYDRACLEAR™ as the ACUVUE® ADVANCE™. Yet, what we have learned about reconditioning gas permeable contact lenses has often been ignored when applied to silicone hydrogel and hydrogel lenses. Although soft lens materials have significant water components, other polymers still create hydrophobic and hydrophilic sites on the lens surface which require surface acting agents to render them more hydrophilic. The best contact lens care products provide lens reconditioning to create long-lasting surface wettability, clean lens surfaces to remove protein or debris and compatible disinfection with safe, effective, non-toxic disinfectants which adequately kill microbial contaminants without compromising corneal surface integrity. This combination of properties collectively improves patient comfort and wearing time.
The patient in this case report failed to realize that her change from a proprietary contact lens care system to a generic PHMB-preserved brand was the cause of her reduction in wearing time and symptoms of dryness and ocular redness. Although a range of possible contributing factors were considered, appropriate and detailed aftercare ultimately resulted in the proper diagnosis and resolution of this patient’s problem. The case report cited highlights the need for detailed and thorough aftercare. Without investigating the cause of this patient’s reduced wearing time and physical discomfort, she and others like her may become another of the many dropouts to contact lens wear.
References:
- Woods CA, Morgan PB. Use of silicone hydrogel contact lenses by Australian optometrists. Clin Exp Optom. 2004 Jan;87(1):19-23.
- Shafer, K. Claims and outcomes of safer, more comfortable contact lens materials. Contact Lens Spectrum. January 2005.
- Stern J, Wong R, Naduvilath TJ, Stretton S, Holden BA, Sweeney DF. Comparison of the performance of 6- or 30-night extended wear schedules with silicone hydrogel lenses over 3 years. Optom Vis Sci. 2004 Jun;81(6):398-406.
- Nilsson SE. Seven-day extended wear and 30-day continuous wear of high oxygen transmissibility soft silicone hydrogel contact lenses: a randomized 1-year study of 504 patients. CLAO J. 2001 Jul;27(3):125-36.
- Lievens CW, Hakim N, Chinn A. The effect of multipurpose solutions on the ocular surface. Eye Contact Lens. 2006 Jan;32(1):8-11.
- Lebow KA, Schachet JL. Evaluation of corneal staining and patient preference with use of three multi-purpose solutions and two brands of soft contact lenses. Eye Contact Lens. 2003;29(4):213-20.
- Jones L, MacDougall N, Sorbara LG. Asymptomatic Corneal Staining with the use of Balafilcon Silicone-hydrogel Contact Lenses Disinfected with Polyaminopropyl Biguanide-preserved Care Regimen. Optom Vis Sci 2002, Dec;79(12):753-61.
- Ketelson HA, Meadows DL, McQueen ND, et. al. Enhancing wettability with multi-purpose solutions. Review of Cornea and Contact Lenses. 2005,1:44-48.
|