It’s often said that there is nothing new under the sun and this certainly seems to be the case with respect to the debate on what should be the required oxygen delivery characteristics during contact lens wear. Currently, there is much interest in establishing the levels of oxygen that exist beneath contact lenses during wear and one common means of estimating this quantity is to measure the oxygen uptake rate (OUR) at the corneal surface immediately upon lens removal. This is by no means a new approach, either technologically or methodologically, and has been visited and revisited many times over the last few decades.
An example of one such visitation appears in a 2000 paper published by Galvin et al. (Galvin KE, Fink B & Hill RM., Oxygen: how well is the cornea being served? Optometry (2000): 71: 239-244.). The intention of this work was to provide clinicians and manufacturers with a view of how the cornea responds to wearing contact lenses having a range of oxygen transmissibility (Dk/t) characteristics and to indicate how this response would vary between the open and closed eye situations.
To carry out these aims, OUR measurements were taken on a small group of subjects who wore each of six RGP lenses having oxygen transmissibilities in the range 0, i.e. PMMA, to 91 x10-9 (cm/sec)(ml O2/ml mmHg). OUR was measured in both open and closed eye environments, with lenses being worn for 5 minutes in each case. Subjects began each session by having open eye OUR measurements taken in the absence of any lenses. This baseline level was used as a reference point and to understand the presentation of data it is important to appreciate that corneal responses during all other situations were normalized to this response. Hence, when reported corneal response values become greater than 1, they represent a relative increase in OUR and correspond to an increased hypoxic load.
When plotted as a function of Dk/t, the ensuing corneal response data were well fitted by the following logarithmic expressions:
Open Eye: y = -0.7279Ln(x) + 4.6812-------------(1)
Closed Eye: y = -0.4732Ln(x) + 4.8656------------(2)
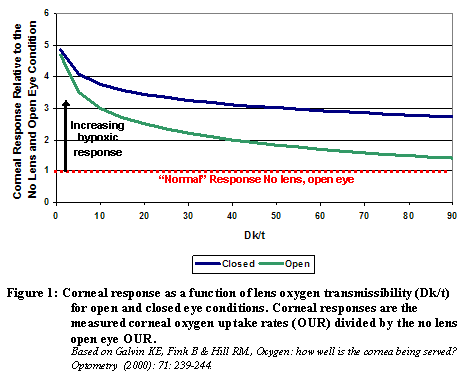
Figure 1 indicates how these curves appear.
In the light of current controversies about critical oxygen levels for the cornea, it is interesting to consider what these results might show us. First of all, the authors offer the suggestion that the shape of the curves indicates that some asymptotic value of maximum hypoxic relief (sic) is being approached at high levels of Dk/t. Although, as they would no doubt have realized, these logarithmic curves do not have asymptotes that lie parallel to the Dk/t axis, it does not alter their interpretation of the effect of the curvature in the data distribution. Hence making incremental increases in Dk/t, in the hope of providing hypoxic relief, will become less and less effective as one moves to progressively higher Dk/t values. In other words, the “bang for the Dk/t buck” is diminished. This so called, “effect of diminishing returns”, has become a widely discussed feature during contemporary debate and commentary on appropriate levels of oxygen transmissibility.
This notwithstanding it is quite clear that none of the lens wearing situations was able to match the corneal response found without lens wear. As is evident from Figure 1, all measured lenses caused relative increases in OUR and the lower the Dk/t, the larger this increase became. Thus, even at a Dk/t of 91 x10-9 (cm/sec)(ml O2/ml mmHg), there was a significant and measurable change in the open eye corneal response relative to no wear.
Not surprisingly, due to the limited availability of oxygen beneath the eyelid, closed eye conditions had a larger impact on OUR at all Dk/t values, than did the open eye state. However, the curves also show how the “hypoxic gap”, or difference in corneal response between the open and closed eye, reduces as Dk/t falls. Thus the cornea is relatively unaffected by lid closure when low Dk/t lenses are worn, because it is already in a substantially hypoxic state.
As in a good novel the authors present us with a final, contemporaneously relevant twist when they raise the concept of maximally effective Dk/t. This is defined as the transmissibility that would produce no change in the corneal response relative to no lens wear. By solving Equation 1 for a corneal response value of y = 1, it would have been possible to produce an estimate for this value. However, perhaps because they were wary of extrapolating beyond their measured data, these workers chose not to take this route. Electing instead to utilize alternative sources of information, they arrived at an estimate for the maximally effective Dk/t of about 350 x10-9 (cm/sec)(ml O2/ml mmHg). This value seems quite high by current standards, and is toward the upper end of the range of estimates available from various other sources. One cannot help but observe that if a corneal response value of 1 were to be inserted into the derived open eye response relationship given above (Equation 1), the maximally effective Dk/t that emerges is rather lower at around 155 x10-9 (cm/sec)(ml O2/ml mmHg). However it is certainly not the intention of this writer to re-interpret Galvin et al.’s data, so in the absence of means to assess the validity of this value I will refrain from further comment.
Galvin et al have reported a piece of work that provides clinicians with useful practical indications for choosing the transmissibility of lenses for both daily and extended wear. With the caveat that they worked exclusively with RGP lenses, so extending their results to cover soft lens behaviour will require some degree of caution, these findings can continue to be of value in informing present day opinion.
|