Manuscript Review
The Measurement of Corneal Epithelial Thickness in Response
to Hypoxia Using Optical Coherence Tomography.
Jianhua Wang, Desmond Fonn, Trefford Simpson, and Lyndon Jones
American Journal of Ophthalmology 2002: Vol 133, No. 3
INTRODUCTION
The corneal stroma has so far been reasonably predictable in
terms of thickness changes in response to hypoxia. The epithelium's
response however has not been consistent between studies (both
short and long-term) and does not appear to be as predictable.
Recent advances in equipment and the introduction of high Dk
lens materials, which allow differentiation between hypoxia
and lens effects, have led to a resurgence of interest in this
area.
HYPOXIC EFFECTS ON STROMAL THICKNESS
Short term studies have firmly established the 5-15% swelling
response of the corneal stroma to hypoxia that is evidenced
clinically by striae when greater than 5% and the additional
presence of folds, when greater than 8% 1.
The classic Gothenburg study by Holden and colleagues showed
thinning of the stroma with long term (62 29 months) wear of
low Dk hydrogel lenses worn on an extended wear (EW) schedule
1. Recent studies have shown a decrease in posterior keratocyte
density in long term EW of low Dk hydrogels that is most likely
responsible for this reduced thickness 2, 3.
UNDISPUTED EFFECTS OF HYPOXIA ON THE EPITHELIUM
Associated with hypoxia, the epithelium exhibits:
- a significant increase in microcysts 4,
- abnormal metabolism that results in an acid shift in pH
due to an accumulation in lactic acid and carbon dioxide 5,
- a reduction in cell synthesis due to enzyme shifts 6,
- reduced epithelial cell adhesion 7,
- increased binding of bacteria to cells 8,
- reduced apoptosis (or programmed cell death) 9
- an increase in cell size 10.
HYPOXIC EFFECTS ON EPITHELIAL THICKNESS: LONG TERM STUDIES
The Gothenburg study showed not only a decrease in stromal
thickness, but also a decrease in epithelial thickness (5.6%
compared to the control eye) with long term (62 29 months) wear
of low Dk hydrogel lenses on an EW schedule. However, this difference
decreased after ceasing lens wear and after 2 days was not significant,
exhibiting recovery of the epithelium 1.
A recent long-term clinical study (over 10 years of low Dk
hydrogel daily lens wear) has not, however, found evidence of
epithelial thinning 11. Possible reasons for this difference
may be less hypoxia with DW compared to EW of low Dk soft lenses,
longer term survival in low Dk hydrogel lens wear of the "fittest"
corneas or possibly a longer term adaptive effect.
HYPOXIC EFFECTS ON EPITHELIAL THICKNESS: SHORT TERM STUDIES
Most of the short-term studies have shown no change in epithelial
thickness 12-15, although there have been several studies on
excised rabbit corneas that have shown an increase in epithelial
thickness with hypoxia 16-18.
THIS STUDY: WHY AND HOW
The purpose of the study was to determine if there was an associated
increase in epithelial thickness with corneal edema induced
by a contact lens worn during eye closure. Twenty subjects wore
thick (0.34-0.41mm) HEMA 38% water content lenses (average Dk/t
of 2.1 x 10-9 on one eye which was patched for 3 hours. The
contralateral eye of each subject, which did not wear a contact
lens and was not patched, acted as the control.
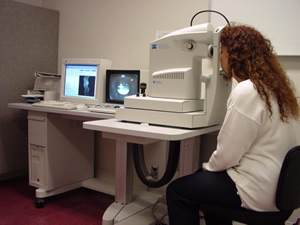 |
| Optical Coherence Tomography
(OCT) setup (Humphrey Instruments, Zeiss-Humphrey, San Leandro,
CA) |
The method used to measure corneal tissue thickness was optical
coherence tomography (OCT) which uses low coherence interferometry
to produce high resolution cross-sectional maps of the anatomical
structure. OCT is similar to ultrasound B-mode imaging, using
light instead of acoustic waves. This is a new optical imaging
technique that was originally designed for measuring different
layers of the retina and has recently been used in several studies
involving measurement of the cornea and the epithelium. Good
reproducibility of OCT measurement of the thickness of the cornea
and epithelium has been previously reported by this group 19.
Other methods to measure the thickness of the cornea include:
-in vivo confocal microscopy through focussing (CMTF) (the confocal
microscope uses the one objective lens to illuminate and focus
a bright spot of light and is thereby able to produce very sharp
images; intensity curves of cell layers are generated and thickness
calculated from the z-axis positions; invasive), and;
-modified optical pachymetry (an optical system that uses two
parallel glass plates to bisect the image of the cornea; measurement
is done by aligning the two images; non invasive but can be
difficult to judge with increased light scatter as in stromal
edema).
THIS STUDY: FINDINGS
For the test eyes, there was a 13.8+/-2.3% increase in overall
corneal thickness and a small (1.7+/-4.8%) but not statistically
significant increase in epithelium thickness. However, there
was slight thinning of the epithelium in the test eye on removal
of the lens (up to 3.0+/-4.5%) over a 100 minute time period.
In addition, the control eye showed a decrease in total corneal
thickness after removal of the contact lens from the test eye,
compared to baseline readings of the control eye.
There was good agreement between the measurements of the test
and control eye and a low standard deviation compared to other
methods of measurement of the corneal epithelium, indicating
good reliability of the OCT for this type of measurement.
THIS STUDY: SIGNIFICANCE OF THE FINDINGS
The increase in total thickness of the cornea falls within
the 5-15% expected range and the small but not statistically
significant increase in epithelium thickness is in line with
the majority of previous short-term studies. It has been previously
suggested that the absence of epithelial swelling may be due
to a compensatory regulatory mechanism contained within the
living epithelium or that radial rather than axial swelling
of the epithelium occurs 12.
Epithelial thinning during the deswelling period has been previously
reported 15 but confirmation of this phenomenon in this study
leads the authors to hypothesize that this may be due to an
auto-regulation effect where the cornea continues to expel fluid
or thins beyond its baseline thickness.
The authors speculate that the corneal thinning of the control
eye may be a sympathetic response. Sympathetic corneal swelling
of the control eye has been previously reported, first by Harris
and Mandell with PMMA 20 and more recently by Fonn et al 21,
comparing the response with both low and high Dk lens wear (the
control eye swelled more when the low Dk, compared to the high
Dk lens was worn on the contralateral eye). Harris and Mandell
proposed that the sympathetic response was due to an osmolarity
effect as a result of lacrimation.
THE STROMA IN HIGH DK EW AND CW
Clinically, striae and folds are rarely seen in high Dk EW
and CW 22.
Recent long term studies have shown a decrease in stromal thickness
and posterior stromal cell density with both long term wear
of low and high Dk material lenses 2, 3. This suggests other
factors other than hypoxia, such as the presence of a contact
lens and lens wear schedules, may be exerting an influence on
stromal thickness.
THE EPITHELIUM IN HIGH DK EW AND CW
Microcyst levels are comparable to no lens wear and remain
consistently low over at least 18 months of high Dk CW for new
lens wearers 23. Patients transferring from low Dk EW to high
Dk CW, show a transitory increase in the first three months
of high Dk lens wear and then a decrease to levels similar to
new high Dk lens wearers and non lens wearers 23.
Decreased bacterial binding of epithelial cells in high Dk
soft lens EW and CW is arguably the most positive finding relating
to the corneal epithelium 24, Article Review-Is
it Time to Give Extended Wear Another Chance.
Dwight Cavanagh's group have also reported a decrease in epithelial
thickness over the first 3 months of EW and CW of high Dk soft
lenses, with adaptive recovery of epithelial thickness in subjects
followed up to 12 months of lens wear . However, these changes
were not as marked as those seen with high Dk RGP CW or low
Dk EW 24.
The same study found an increase in the size of the corneal
epithelial cells, however Stapleton et al have found no increase
in epithelial cell size after 3months of CW of high Dk soft
lenses 25.
The effect of long-term contact lens wear on epithelial thickness
appears to be driven by not only hypoxia but also lens effects,
as occurs with the corneal stroma.
CONCLUSION
Results with high Dk lenses are certainly positive. Research
continues into the effects of hypoxia and contact lens wear,
particularly high Dk EW and CW, on the corneal epithelium and
the implications of these changes. New instrumentation such
as the OCT has contributed to the surge in interest in this
area and it will be interesting to see the results of long-term
clinical studies with these new methods of measurement.
1. Holden BA, Sweeney DF, Vannas A, Nilsson K, Efron N. Effects
of long-term extended contact lens wear on the human cornea.
Invest Ophthalmol Vis Sci 1985;26:1489-1501.
2. Jalbert I, Stapleton F. Effect of lens wear on corneal stroma:
preliminary findings. Australian & New Zealand Journal of
Ophthalmology 1999;27(3-4):211-3.
3. Perez-Gomez I, Morgan P, Efron N. Confocal microscopic appearance
and thickness of the cornea following extended wear contact
lenses: a study with neophytes. Optom. Vis. Sci. 2001;78(12s):199.
4. Zantos SG, Holden BA. Ocular changes associated with continuous
wear of contact lenses. Aust J Optom 1978;61:418-426.
5. Klyce SD. Stromal lactate accumulation can account for corneal
oedema osmotically following epithelial hypoxia in the rabbit.
J Physiol 1981;321:49-64.
6. Fullard RJ, Carney LG. Human tear enzyme changes as indicators
of the corneal response to anterior hypoxia. Acta Ophthalmologica
1985;63(6):678-83.
7. Madigan MC, Holden BA, Kwok LS. Extended wear of contact
lenses can compromise corneal epithelial. Current Eye Research
1987;6(10):1257-60.
8. Ren DH, Petroll WM, Jester JV, Ho-Fan J, Cavanagh HD. The
relationship between contact lens oxygen permeability and binding
of Pseudomonas aeruginosa to human corneal epithelial cells
after overnight and extended wear. CLAO J 1999;25:80-100.
9. Yamamoto K, Ladage PM, Ren DH, Li L, Petroll WM, Jester JV,
et al. Effects of low and hyper Dk rigid gas permeable contact
lenses on Bcl-2 expression and apoptosis in the rabbit corneal
epithelium. CLAO Journal|CLAO (Contact Lens Association of Ophthalmologists)
Journal 2001;27(3):137-43.
10. Lemp MA, Gold JB. The effects of extended-wear hydrophilic
contact lenses on the human corneal epithelium. American Journal
of Ophthalmology 1986;101(3):274-7.
11. Bourne W. The effect of long-term contact lens wear on the
cells of the cornea. CLAO J 2001;27(4):225-30.
12. Lambert SR, Klyce SD. The origins of Sattler's veil. American
Journal of Ophthalmology 1981;91(1):51-6.
13. Wilson G, Fatt I. Thickness of the corneal epithelium during
anoxia. American Journal of Optometry & Physiological Optics
1980;57(7):409-12.
14. Bergmanson JP, Ruben CM, Chu LW. Epithelial morphological
response to soft hydrogel contact lenses. British Journal of
Ophthalmology|The British Journal of Ophthalmology 1985;69(5):373-9.
15. O'Leary DJ, Wilson G, Henson DB. The effect of anoxia on
the human corneal epithelium. American Journal of Optometry
& Physiological Optics 1981;58(6):472-6.
16. Uniacke CA, Hill RM. The depletion course of epithelial
glycogen with corneal anoxia. Archives of Ophthalmology 1972;87(1):56-9.
17. Lowther GE, Hill RM. Recovery of the corneal epithelium
after a period of anoxia. American Journal of Optometry &
Archives of American Academy of Optometry 1973;50(3):234-41.
18. Uniacke CA, Augsburger A, Hill RM. Epithelial swelling with
oxygen insufficiency. American Journal of Optometry & Archives
of American Academy of Optometry 1971;48(7):565-8.
19. Fonn D, Wang J, Simpson T. Topographical thickness of the
epithelium and total cornea using optical coherence tomography.
Invest Ophthalmol Vis Sci 2000;41(S675).
20. Harris M, Mandell R. Contact lens adaptation: osmotic theory.
Am J Ophthalmol 1969;46:196-202.
21. Fonn D, du Toit R, Situ P, Vega JA, Simpson T, Chamlers
R. Apparent sympathetic response of contralateral nonlens wearing
eyes after overnight lens wear in the fellow eye. [ARVO Abstract].
Invest Ophthalmol Vis Sci 1998;39:S336.
22. Covey M, Sweeney DF, Terry RL, Sankaridurg PR, Holden BA.
Hypoxic effects on the anterior eye of high Dk soft contact
lens wearers are negligible. Optom Vis Sci 2001;78:95-99.
23. Keay L, Sweeney DF, Jalbert I, Skotnitsky C, Holden BA.
The microcyst response to high Dk/t silicone hydrogel contact
lenses. Optom Vis Sci 2000;77:582-585.
24. Ren DH, Yamamoto K, Ladage PM, Molai M, Li L, Petroll WM,
et al. Adaptive effects of 30-night wear of hyper-O(2) transmissible
contact lenses on bacterial binding and corneal epithelium:
a 1-year clinical trial. Ophthalmology 2002;109(1):27-39; discussion
39-40.
25. Stapleton F, Kasses S, Bolis S, Keay L. Short term wear
of high Dk soft contact lenses does not alter corneal epithelial
cell size or viability. Br J Ophthalmol 2001;85:143-146.