Mucin Balls….I always think they are a bit like the Hilton
sisters, Paris and Nikki……. everyone has seen them,
no-one is particularly impressed, but you vaguely wish they’d
go away! These round, translucent or opalescent bodies (Figure
1) can be seen trapped in the space between the contact lens
and cornea and are usually around 50µm
in diameter, though size can vary between about 20 and 200µm.
While much more common among
wearers of silicone hydrogel lenses, individual susceptibility
varies substantially.
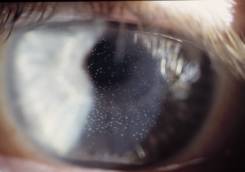 |
| Figure
1: Contact lens wearer displaying large
numbers of mucin balls |
In assessing the significance of these features,
the first task for the clinician is to make sure that they are
indeed looking
at mucin balls, rather than the features with which they are
most commonly confused, namely microcysts or vacuoles. Among
the signs to look for when making the differential diagnosis
are that mucin balls have a pre-epithelial location, and will
usually disappear within a few blinks after lens removal. Both
microcysts and vacuoles are intra-epithelial, and persist when
the lens is removed. If doubt still remains, instillation of
sodium fluorescein will show pooling of the dye (though not frank
staining), in the epithelial depressions left behind by the mucin
ball (Table 1). This appearance is similar to “dimple
veiling”, which was caused by bubbles of gas collecting
beneath rigid lenses.
Mucin Balls
|
Microcysts
|
Vacuoles
|
Abolished on lens removal
|
Persist on lens removal
|
Translucent
|
Reversed Illumination
|
Unreversed Illumination
|
NaFL pooling in depression
|
Occasional NaFl stain
|
No NaFl stain
|
|
| Table
1: Differential diagnosis of mucin balls |
Our knowledge of the nature of
mucin balls has improved recently as samples have been collected
and subjected to scanning electron microscopy, histochemistry
and other analytical techniques.3 These studies have shown it
to be quite unlikely that mucin balls have been misnamed, which
is to say that their major constituent does indeed appear to
be mucin! Presumably, this material is derived from the pre-ocular
tear film and is formed into spheroids by the relative motion
between the contact lens and corneal surface. Consequently, it
has been proposed that reducing this motion, by more closely
matching lens shape to that of the ocular surface, would be a
possible means of cutting down mucin ball numbers.1
Despite being squeezed between the contact lens and epithelium,
mucin balls tend to maintain their spherical shape. This resistance
to deformation is responsible for creating the epithelial depressions
and these may be quite deep. When viewed with the confocal microscope,
the indentations can often be seen extending at least to the
level of Bowman’s membrane4, and possibly even beyond.5
In these circumstances one might reasonably wonder what happens
to the corneal cells immediately beneath a mucin ball? So far,
it has proved difficult to visualize epithelial cells in this
region; suggesting either, that they have become highly compacted,
or possibly that migration away from the local pressure point
has occurred. Interestingly, a similar conundrum currently surrounds
the mechanisms of epithelial remodeling during orthokeratology,
and in that case, recent data tend to favour the compaction theory.6
With respect to stromal tissue, indications from rabbit eyes
are that the keratocytes or fibroblasts underneath deeper mucin
ball impressions show signs of increasing their proliferation
rate.4 The significance of this finding currently remains unclear,
though stromal cells usually divide rather slowly.
While evidence of cellular activity in the cornea is certainly
a good reason for continued research, from the viewpoint of both
clinician and wearer, it is comforting that there have been almost
no reports of associated negative clinical events. This is despite
the fact that mucin balls are highly prevalent among silicone
hydrogel wearers. Apart from a statistical indication that extended
wearers with larger numbers may have a slightly increased risk
(x 1.7) of developing a contact lens induced peripheral ulcer
(CLPU),7 mucin ball related adverse events have not featured in
the literature. As there are generally no adverse effects on
either vision or subjective comfort,1, 8, clinical intervention
is usually unnecessary in cases where mucin balls are the only
observable complication. Naturally however, continued, regular
review is recommended throughout the period of contact lens wear.
- Dumbleton K, Jones L, Chalmers R, Williams-Lyn D, Fonn D. Clinical
characterization of spherical post-lens debris associated with
lotrafilcon high-Dk silicone lenses. CLAO J. 2000; 26:186-92.
- Sweeney DF, du Toit R, Keay L, Jalbert I, Sankaridurk PR,
Stern J, Skotnitsky C, Stephensen A, Covey M, Holden BA & Rao
G. Clinical performance of silicone hydrogel lenses. In: Silicone
Hydrogels, continuous wear contact lenses. Ed: Sweeney DF.
2nd
Edition, Butterworth Heinemann. p 198.
- Miller TJ, Papas EB, Ozkan J, Jalbert I & Ball M. Clinical
Appearance and Microscopic
Analysis of Mucin Balls Associated with Contact Lens Wear.
Cornea, 2003, 22,, 740-745.
- Ladage PM, Petroll WM, Jester JV, Fisher S, Bergmanson JPG,
Cavanagh HD. Spherical indentations of human and rabbit corneal
epithelium following extended contact lens wear. CLAO
J. 2002; 28:177-180.
- Jalbert I, Stapleton F, Papas E, Sweeney DF & Coroneo
M. In vivo confocal microscopy of the human cornea. Brit.
J. Ophthalmol. 2003; 87: 225-236.
- Choo J, Caroline PJ, Harlin DD & Myers W. Morphological
changes in the cat epithelium following overnight lens wear
with the Paragon CRT for corneal reshaping. Invest Ophthalmol.
Vis.
Sci. 2004, 45, Abstract 1552.
- Naduvilath TJ. Statistical modeling of risk factors associated
with soft contact lens related corneal infiltrative events.
PhD Thesis (Newcastle: University of Newcastle), 2003.
- Morgan PB & Efron N. Comparitive clinical performance
of two silicone hydrogel contact lenses for continuous wear.
Clin
Exp Optom., 2002; 85, 183-192.
|